“Physician, heal thyself” – but what happens when the healer is drowning in silence?
Sarah sat in the back row of her pharmacology lecture, mechanically taking notes while her mind spiraled into familiar territory. The material felt insurmountable, her latest exam score was disappointing, and she couldn’t shake the feeling that everyone around her was somehow more capable, more deserving of their white coat. What she didn’t realize was that nearly one in three of her classmates was experiencing similar thoughts – trapped in a cycle of perfectionism, comparison, and overwhelming pressure that has created a mental health crisis hiding in plain sight within medical education.
The statistics are both shocking and undeniable. While approximately 8% of the general population experiences depression, studies consistently show that 27% of medical students struggle with depressive symptoms – more than triple the rate of their peers. But the mental health crisis extends far beyond depression alone.
When we examine anxiety disorders, the picture becomes even more alarming. Research reveals that anxiety rates among medical students fluctuate dramatically throughout their education, creating a rollercoaster of psychological distress that tracks with the academic calendar. One comprehensive study found that anxiety affects 45.86% of first-year students, peaks at 52.58% in second year, remains elevated at 47.14% in third year, drops to 28.75% in fourth year, then rises again to 45.10% in the final year.
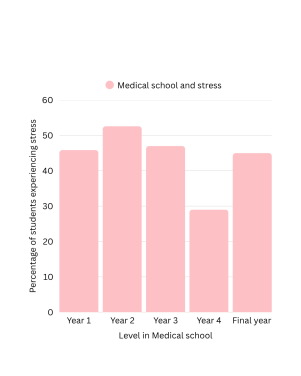
These fluctuations tell a story of how different phases of medical education create unique psychological pressures. The initial shock of medical school intensity hits first-years hard, while second-year students face the notorious “pre-clinical to clinical” transition anxiety. Third-year students grapple with their first real patient responsibilities, fourth-years experience some relief as they near graduation, and final-year students face the stress of residency matching and career uncertainty.
The very individuals we’re training to heal others are experiencing mental health challenges at rates that would constitute a public health emergency in any other population.
The International Journal of Medical Education published a comprehensive meta-analysis in 2019 that examined 77 studies across different countries and cultures. The findings were consistent across geographic boundaries: medical students worldwide experience depression at rates 2.5 to 3 times higher than age-matched peers in other fields.
Why are so many medical students depressed?
The answer lies in a convergence of factors that create the perfect storm for mental health struggles. Medical students face a unique combination of extreme academic pressure, high-stakes testing, financial stress from significant debt, social isolation due to demanding schedules, and the psychological burden of preparing to hold lives in their hands.
Why do medical students have anxiety?
The anxiety epidemic stems from the uncertainty inherent in medical training. Students constantly face the unknown – will they pass their next exam? Will they match into their desired residency? Can they handle the responsibility of patient care? This chronic uncertainty, combined with perfectionist tendencies, creates persistent anxiety that can become debilitating.
Why are students more prone to depression?
Medical students are particularly vulnerable because they enter medical school as high achievers who have rarely experienced failure. When they encounter the normal struggles of medical education, they lack coping mechanisms for anything less than perfection. Additionally, the isolation from friends and family, financial pressures, and constant evaluation create a breeding ground for depressive symptoms.
What is the most stressful year of medical school? Based on anxiety data, second year emerges as the most psychologically challenging, with anxiety rates reaching 52.58%. This year combines intense studying for the first major licensing exam (USMLE Step 1) with the pressure of transitioning from basic sciences to clinical application – a combination that overwhelms more than half of all students.
Medical school attracts individuals who have spent their entire academic careers at the top of their class. These are students who have never encountered failure, who have built their identity around being the best, the brightest, the most capable. Then they enter medical school, where suddenly everyone is exceptionally talented.
Dr. Lisa Rotenstein, who has extensively researched medical student mental health, explains that this shift from being a big fish in a small pond to being surrounded by equally accomplished peers creates what psychologists call “the big fish-little pond effect.” For many students, this is their first encounter with academic struggle, and they lack the coping mechanisms to handle anything less than excellence.
The perfectionism that once served as a driving force becomes a destructive inner critic. Students begin to catastrophize normal academic challenges, viewing a single poor grade as evidence of their unworthiness to become a physician. This all-or-nothing thinking pattern, combined with the high stakes of medical education, creates a breeding ground for anxiety and depression.
The Imposter Syndrome Epidemic
“I don’t belong here.” “They made a mistake accepting me.” “Everyone else seems to understand this better than I do.” These thoughts plague medical students at alarming rates, creating what psychologists term “imposter syndrome” – the persistent feeling of being a fraud despite evidence of competence.
Medical education, with its emphasis on extensive knowledge and life-or-death decision-making, naturally amplifies these feelings. Students compare their internal struggles with their peers’ external composure, not realizing that everyone is fighting similar battles. The competitive atmosphere often discourages vulnerability and honest communication about difficulties, perpetuating the illusion that everyone else is managing better.
Maya, a third-year medical student, shared her experience: “I spent my first two years convinced that admissions had made an error. Every time I didn’t know an answer during rounds, I was sure my attending would realize I didn’t deserve to be there. It wasn’t until I started opening up to classmates that I realized we were all feeling the same way.”
Academic Pressure and the Stakes of Failure
Unlike other graduate programs, medical school carries the weight of future patient care. Students aren’t just worried about their GPA – they’re concerned that their academic performance directly correlates with their ability to save lives. This creates a unique psychological pressure that goes beyond normal academic stress.
The USMLE Step exams, residency applications, and clinical rotations all carry high stakes that can determine career trajectories. Students often report feeling that a single poor performance could derail their entire future, leading to chronic stress and anxiety that compounds over time.
Breaking the Stigma
Perhaps the most insidious aspect of this mental health crisis is the culture of silence that surrounds it. Medical students often fear that seeking help will be seen as weakness, that it will be documented in their records, or that it will prevent them from matching into competitive residencies.
This fear isn’t entirely unfounded. While progress has been made, some residency programs still ask about mental health history, and students worry about the implications of being honest about their struggles. The result is a culture where suffering in silence is normalized, where students push through depression and anxiety without seeking the help they desperately need.
Dr. Pamela Wible, a physician advocate for medical professionals’ mental health, describes this as “medical training trauma” – the normalization of abuse, neglect, and suffering as necessary components of becoming a physician. This toxic culture suggests that struggling with mental health indicates weakness or unsuitability for medicine, when in reality, it’s a natural human response to an unnaturally stressful environment.
Recognizing the Warning Signs
The tragedy of medical student mental health crises is that they’re often preventable with early recognition and intervention. Understanding the warning signs – both for oneself and for classmates – can be life-saving.
Physical symptoms often appear first: changes in sleep patterns, appetite fluctuations, frequent headaches, or unexplained fatigue. These may be dismissed as normal stress responses, but they often signal the beginning of more serious mental health challenges.
Cognitive changes include difficulty concentrating, memory problems, indecisiveness, or persistent negative thoughts. Students might notice that material that once came easily now feels impossible to grasp, or that they’re spending significantly more time studying with less retention.
Emotional indicators encompass feelings of hopelessness, excessive guilt, irritability, or emotional numbness. Some students report feeling like they’re “going through the motions” without experiencing genuine emotions.
Behavioral changes might include social withdrawal, neglecting self-care, increased substance use, or avoiding previously enjoyable activities. Students might stop exercising, eating poorly, or isolating themselves from friends and family.
Recognizing Signs in Classmates
Medical students often notice changes in their peers before recognizing them in themselves. Warning signs in classmates include dramatic changes in academic performance, increased absence from class or clinical rotations, social withdrawal, or comments about feeling hopeless or worthless.
The phrase “I’m just tired” becomes a common refrain that often masks deeper struggles. Students might joke about wanting to “disappear” or make offhand comments about not being cut out for medicine. These seemingly casual remarks often reflect genuine distress.
How Mental Health Impacts Medical Education
The consequences of untreated mental health issues extend far beyond individual suffering. Depression and anxiety significantly impact academic performance, with studies showing that medical students with untreated mental health conditions are more likely to struggle academically, drop out, or experience difficulties during clinical rotations.
More concerning is the impact on patient care. Students struggling with mental health issues report feeling less empathetic toward patients, making more medical errors, and experiencing greater difficulty with clinical decision-making. This creates a dangerous cycle where poor mental health leads to compromised patient care, which in turn increases guilt and worsens mental health symptoms.
The financial implications are also substantial. Medical education represents a significant investment, and mental health struggles can lead to academic delays, repeated coursework, or even withdrawal from medical school. The average medical student graduates with debt, making the consequences of mental health-related academic difficulties particularly devastating.
A Call for Change
Addressing the mental health crisis in medical education requires more than individual intervention. Medical schools are beginning to recognize this, implementing wellness curricula, providing mental health resources, and working to reduce stigma.
However, true change requires a fundamental shift in medical education culture. We must move away from the idea that suffering is necessary for becoming a good physician and toward a model that prioritizes well-being as essential for providing excellent patient care.
Students themselves play a crucial role in this cultural shift. By speaking openly about mental health struggles, supporting classmates, and prioritizing self-care, medical students can help create a more supportive environment for everyone.
The key is recognizing that seeking help for mental health struggles isn’t a sign of weakness – it’s a sign of strength and wisdom. Just as we wouldn’t expect someone to perform surgery with a broken hand, we shouldn’t expect students to navigate the challenges of medical education with untreated mental health conditions.
Resources and Next Steps
If you’re a medical student struggling with mental health issues, know that you’re not alone and that help is available. Most medical schools offer confidential counseling services, and many have specific programs designed for medical students.
Remember that seeking help early is always better than waiting until the situation becomes critical. Mental health treatment is not a luxury, it’s an essential component of your medical education and future practice.
Conclusion
The mental health crisis among medical students represents one of the most pressing challenges in medical education today. With depression rates three times higher than the general population, we can no longer afford to ignore this issue or dismiss it as a normal part of medical training.
By understanding the root causes – perfectionism, imposter syndrome, and overwhelming academic pressure – and recognizing the warning signs early, we can begin to address this crisis. More importantly, we can work to create a culture in medical education that values mental health as much as academic achievement.
If you’re struggling with mental health issues, please reach out for help. You deserve support, and seeking help makes you a better future physician, not a weaker one.
Sources:
- Rotenstein, L. S., et al. (2016). Prevalence of depression, depressive symptoms, and suicidal ideation among medical students. JAMA, 316(21), 2214-2236.
- Pacheco, J. P., et al. (2019). Mental health problems among medical students in Brazil. International Journal of Medical Education, 10, 224-230.
- Dyrbye, L. N., et al. (2014). Burnout and suicidal ideation among U.S. medical students. Annals of Internal Medicine, 149(5), 334-341.
- Mirza AA, Baig M, Beyari GM, Halawani MA, Mirza AA. Depression and Anxiety Among Medical Students: A Brief Overview. Adv Med Educ Pract. 2021 Apr 21;12:393-398. doi: 10.2147/AMEP.S302897. PMID: 33911913; PMCID: PMC8071692.