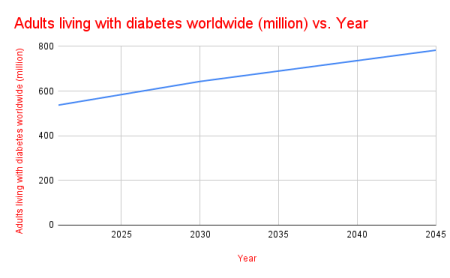
Over 537 million adults (20–79 years) were living with diabetes worldwide in 2021. That number is projected to rise to 643 million by 2030 and 783 million by 2045.
Diabetes is one of the most common chronic conditions in the world today. It affects how your body turns food into energy. It happens when your blood sugar levels are too high because your body either doesn’t make enough insulin or can’t use it well. Insulin is a hormone that helps glucose from food get into your cells to be used for energy. When this process doesn’t work properly, sugar stays in your bloodstream. Over time, diabetes can lead to serious health issues.
What Is Diabetes?
At its core, diabetes is a condition that affects how your body processes blood sugar (glucose). There are several types of diabetes. Type 1 diabetes is an autoimmune condition where the body attacks the insulin-producing cells in the pancreas. Type 2 diabetes, the most common type, happens when the body becomes resistant to insulin or doesn’t produce enough of it. Gestational diabetes occurs during pregnancy and usually goes away after childbirth, but it increases the risk of developing Type 2 diabetes later. Other,less common forms of diabetes can also occur due to genetic conditions, medications, or diseases of the pancreas.




Common Symptoms of Diabetes
Symptoms of diabetes can be subtle at first, especially with Type 2 diabetes. However, some early warning signs can help you catch it before complications arise. These include:
- Frequent urination
- Extreme thirst
- Unexplained weight loss
- Increased hunger
Other signs you might notice include darker patches of skin on the neck (a condition called acanthosis nigricans), recurring infections (especially urinary or skin), blurred vision, and even sexual dysfunction. Some people experience pain, tingling, or numbness in their hands or feet—this is a sign that diabetes may be affecting the nerves.
When Should You See a Doctor?
If you’re experiencing any of these symptoms—especially more than one—it’s a good idea to talk to a doctor. Even if you’re not showing obvious signs, routine screening is recommended if you’re over 45 or have risk factors such as being overweight, having a family history of diabetes, or living a sedentary lifestyle. Diabetes is diagnosed through blood tests like the A1C test, fasting blood sugar test, or an oral glucose tolerance test.
Understanding Risk Factors
Some risk factors for Type 2 diabetes are beyond your control, such as age, ethnicity, and family history. However, many risk factors are related to lifestyle, including physical inactivity, poor diet, high blood pressure, and excess weight—especially fat around the abdomen. Stress can also play a role, as chronic stress may raise blood sugar levels and make insulin resistance worse.
Living with Diabetes
Diabetes doesn’t just affect your blood sugar; it impacts nearly every part of your life. It can affect how you feel day to day, limit what you eat, and even cause emotional distress. But with the right knowledge and habits, many people with diabetes live long, active, and fulfilling lives. Managing diabetes means making smart food choices, staying physically active, monitoring your blood sugar levels, and sometimes taking medication or insulin.
Myths and Misconceptions
One of the most common myths is that eating too much sugar directly causes diabetes. While diet does play a role, it’s more about the overall pattern of eating, lifestyle, and genetics. Another myth is that only overweight people get diabetes—while weight is a risk factor, many people of normal weight also develop the condition. And no, diabetes is not contagious, and it can’t be cured with home remedies or “detoxes.”
Complications of Diabetes
If left untreated or poorly managed, diabetes can lead to serious complications. These include:
- Heart disease
- Kidney failure
- Vision loss
- Nerve damage
- Limb amputations
The major problem with diabetes is not just high blood sugar, but the damage it can do quietly over time to major organs. This is why managing it well and catching it early is so important.
Prevention and Early Action
The good news is that Type 2 diabetes is often preventable. A healthy diet, regular physical activity, maintaining a healthy weight, and managing stress can go a long way in lowering your risk. If you’ve been told you have prediabetes—meaning your blood sugar is higher than normal but not high enough to be diabetes—it’s a sign to act now. Making small lifestyle changes can help you avoid full-blown diabetes and even reverse prediabetes.
Treating and Managing Diabetes
There’s no one-size-fits-all treatment, but diabetes can be managed effectively. This often involves a combination of medication, insulin (for some people), diet changes, and exercise. Some people can manage their diabetes without medication through lifestyle changes alone, especially if it’s caught early. Regular monitoring is key to staying in control.
Eating Right for Diabetes
A good diabetic diet focuses on whole foods like vegetables, lean proteins, whole grains, and healthy fats. Portion control and timing your meals can also help manage blood sugar levels. Foods to avoid or limit include sugary drinks, processed snacks, and refined carbohydrates. Working with a nutritionist can be incredibly helpful.
Stages and Progression
Diabetes doesn’t develop overnight. The four stages include insulin resistance, prediabetes, early Type 2 diabetes, and more advanced diabetes with complications. Knowing these stages can help you catch and manage the condition early, potentially avoiding the more serious effects altogether.
Conclusion
Diabetes is a serious condition, but it’s also manageable—and often preventable. With early detection, lifestyle changes, and the right medical support, you can take control of your health and live well. Don’t wait until symptoms become severe. If you’re at risk or experiencing signs, speak to a doctor. Your future self will thank you.